Dr Cox has subspecialty fellowship training in hip surgery including
- Primary total hip replacement
- Revision hip replacement and infection
- Hip fractures
- Proximal hamstring avulsions
- Assessment of labral pathology
Dr Cox has subspecialty fellowship training in hip surgery including
Osteoarthritis is the destructive process in which joint cartilage wears out, leaving the bones rubbing directly on each other. This is associated with variable degrees of pain and stiffness. Joint replacement (arthroplasty) surgery involves cutting away worn out bone and cartilage and replacing those articulating surfaces with a combination of metallic hip implants, highly specialised plastic (polyethylene) and ceramic bearings.
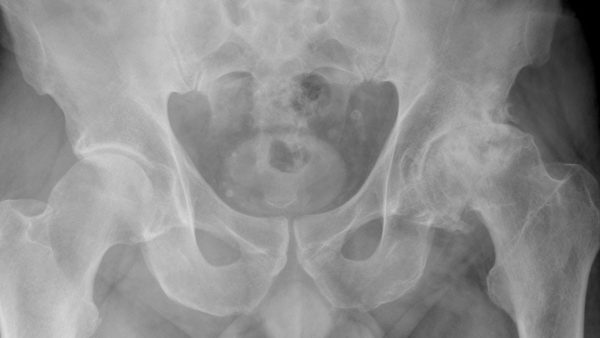 The primary indication for hip replacement surgery is painful advanced arthritis. This pain is usually felt in the groin and deep in the buttock. It is a common procedure with the vast majority of patients reporting improved pain and function after their recovery. However, each patient must weigh these potential benefits against the risks (which include infection, dislocation, implant loosening, persistent pain and medical complications).
The primary indication for hip replacement surgery is painful advanced arthritis. This pain is usually felt in the groin and deep in the buttock. It is a common procedure with the vast majority of patients reporting improved pain and function after their recovery. However, each patient must weigh these potential benefits against the risks (which include infection, dislocation, implant loosening, persistent pain and medical complications).
The hip is essentially a simple ball and socket joint. The “socket” is part of the pelvis and known as the acetabulum. The “ball” is the rounded end of the thigh (femur) bone and known as the femoral head. To the support the femoral head implant, a “femoral stem” is first inserted into the proximal femur then the femoral head component is attached. Total hip replacement involves replacing both the acetabulum and femoral head components with an associated femoral stem. Dr Cox usually uses a hybrid technique which involves an uncemented metal acetabular socket into which a highly specialised “plastic” (cross linked polyethylene) liner is added. This is combined with a cemented femoral stem with a highly polished ceramic femoral head.
Modern hip replacement is a very successful operation with high rates of patient satisfaction and a low complication rate. Two important factors that affect the long-term survivorship of hip replacement for osteoarthritis are experience with the surgical technique and the use of well performing implants. The cumulative revision rate of THR for osteoarthritis using Dr Cox’s preferred implants in Australia is 4% at 10yrs, and 6% at 15yrs.
 Historically, hip replacements were quite unstable, so extreme measures were often recommended until the surrounding scar had time to mature. This has been improved with modern implants (with larger ball and socket bearings) and with modern techniques (tendons are often left intact or repaired during the operation) so that the dislocation rate after routine hip replacement is now less than 1%. Hip precautions after routine modern hip replacement are therefore minimal and by 4 weeks you may be walking without crutches and able to drive a car.
Historically, hip replacements were quite unstable, so extreme measures were often recommended until the surrounding scar had time to mature. This has been improved with modern implants (with larger ball and socket bearings) and with modern techniques (tendons are often left intact or repaired during the operation) so that the dislocation rate after routine hip replacement is now less than 1%. Hip precautions after routine modern hip replacement are therefore minimal and by 4 weeks you may be walking without crutches and able to drive a car.
Whilst hip replacements are very successful, they do not last forever. Unlike the normal hip, the mechanical components of a hip replacement have no capacity for repair, and so will wear out over time. Unfortunately, the wear particles generated stimulate an inflammatory reaction in the body, which leads to loosening of the implants in the bone. This is known as aseptic loosening and is associated with pain which often requires revision. Other causes for revision include infection (either soon after or years after the original surgery), instability, impingement, leg length discrepancy, adverse metal debris reaction or injury.
Revision surgery is more complex than primary hip replacement. Issues to consider include previous scars, bone loss, weakened muscles and tendons, deformity and the removal of failing implants. It has a higher complication rate than primary surgery and so only significant pain and dysfunction justify the risks. Despite these risks, a good outcome can be expected in most cases as long as a careful approach is taken to preoperative workup and surgical technique.
Hip fractures usually occur in older patients following a fall from standing height. The fracture can occur through the neck of femur (“nof”) or the trochanteric region (intertrochanteric). In most cases, intertrochanteric fractures are managed with surgical fixation (commonly a short femoral nail) whilst displaced fractures through the neck are managed with hip replacement. This can be either total or hemiarthroplasty. Hemi (“half”) relates to replacing the femoral head (“ball”) component whilst leaving the patient’s acetabulum (“socket”) alone. Many patients do well with total hip arthroplasty, but the lower complexity and favourable risk profile of hemiarthroplasty justifies its use in the particularly elderly or low demand patients.
 Because of the unplanned nature of hip fracture surgery and the significant medical comorbidities common in this patient group, other specialists from Internal Medicine, Geriatrics and Rehabilitation are often actively involved in the acute and ongoing care of these patients.
Because of the unplanned nature of hip fracture surgery and the significant medical comorbidities common in this patient group, other specialists from Internal Medicine, Geriatrics and Rehabilitation are often actively involved in the acute and ongoing care of these patients.
The hamstrings are a group of muscles in the back of the thigh (biceps femoris, semimembranosus and semitendinosus). They attach proximally to the ischial tuberosity (the part of the pelvis bone you sit on) and split to attach distally on both sides of the leg just below the knee joint. Mid-substance (muscle belly or musculotendinous junction) injuries are a very common sporting injury and respond very well to non-operative therapy with light activity until pain settles. Proximal hamstring avulsions however, involve the tendon ripping off the ischial tuberosity attachment on the pelvis, sometimes with a small flake of bone torn off too. These injuries have less healing capacity and so are often fixed surgically in high demand patients. This involves reattaching the tendons with suture anchors into the bone and protecting the repair whilst it heals. The risks include re-rupture and injury to the sciatic nerve. Complications are rare in acute repairs (within 3 weeks) but increase with delayed repairs because scar tissue makes the surgery more difficult.
 The labrum is a specialised type of fibrocartilage that attaches around the rim of the acetabulum (“socket”). It helps to functionally deepen the socket and stabilise the femoral head. At the extremes of hip movement, the femoral neck contacts the labrum, which can lead to repetitive microtrauma. This can progress to a degenerate labral tear. In the absence of significant arthritis, the symptoms are often well tolerated with simple analgesia, activity modification and directed physiotherapy. If associated with significant arthritis, then the labral findings are secondary and the hip arthritis itself should be managed accordingly depending on severity (often with total hip replacement). Occasionally, acute tears occur in young people with an otherwise normal labrum. In this patient group hip arthroscopy surgery can be helpful to repair the tear.
The labrum is a specialised type of fibrocartilage that attaches around the rim of the acetabulum (“socket”). It helps to functionally deepen the socket and stabilise the femoral head. At the extremes of hip movement, the femoral neck contacts the labrum, which can lead to repetitive microtrauma. This can progress to a degenerate labral tear. In the absence of significant arthritis, the symptoms are often well tolerated with simple analgesia, activity modification and directed physiotherapy. If associated with significant arthritis, then the labral findings are secondary and the hip arthritis itself should be managed accordingly depending on severity (often with total hip replacement). Occasionally, acute tears occur in young people with an otherwise normal labrum. In this patient group hip arthroscopy surgery can be helpful to repair the tear.